Probably drug-induced toxic epidermal necrolysis in an adolescent.
Downloads
DOI:
https://doi.org/10.26326/2281-9649.36.2.2899How to Cite
Abstract
Toxic epidermal necrolysis (TEN) is a rare, life-threatening mucocutaneous adverse reaction, most commonly triggered by medications. Although uncommon in children and adolescents, TEN carries significant morbidity and mortality, requiring prompt diagnosis and multidisciplinary management.
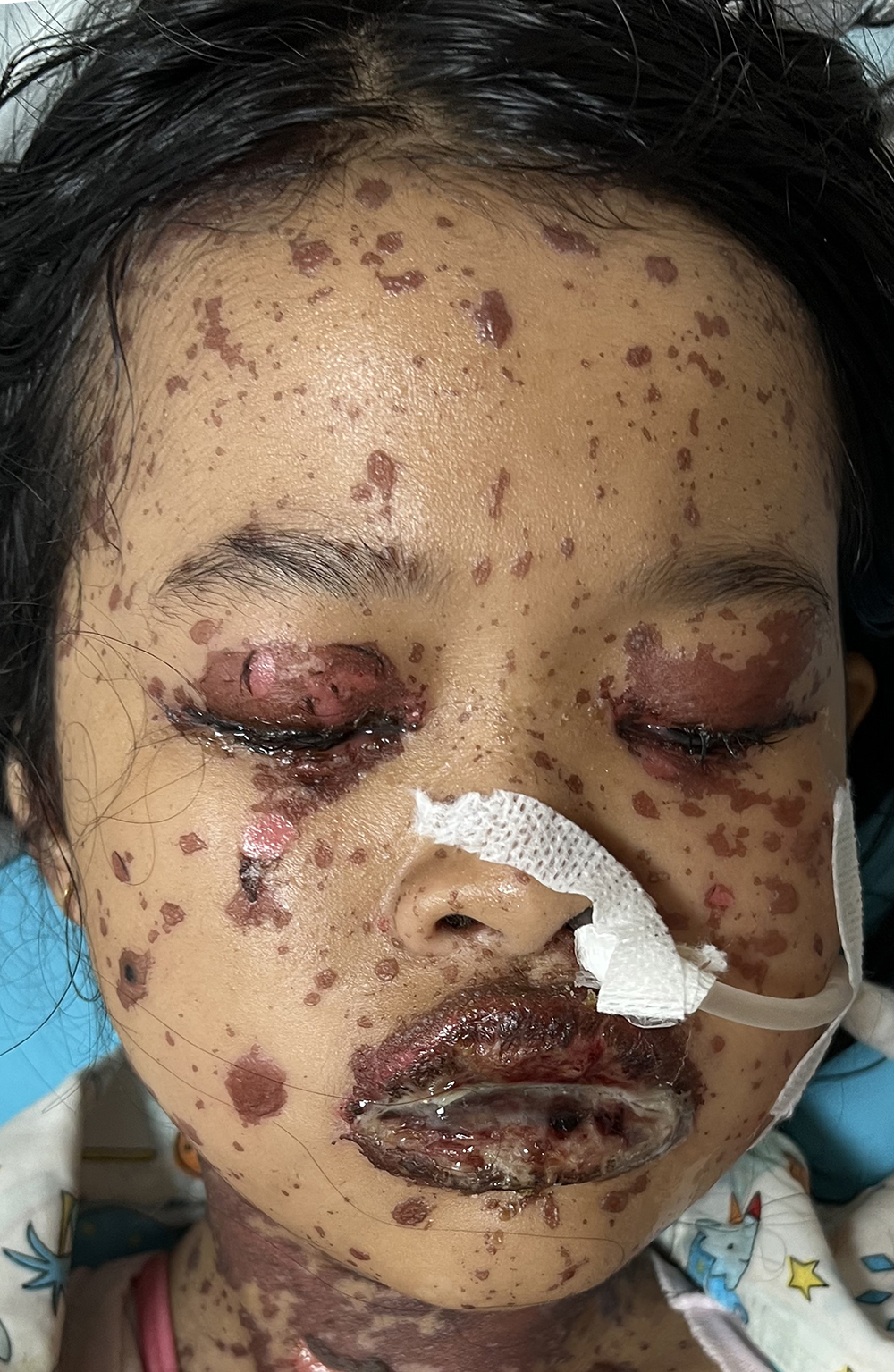
This work aims to report a diagnostic challenge case of drug-induced TEN in an adolescent and to highlight the importance of early recognition and timely intervention in achieving favorable outcomes. A 13-year-old girl developed persistent high-grade fever followed by rapidly progressive generalized erythematous-to-dusky macules evolving into extensive epidermal detachment involving more than 90% of the total body surface area. Severe mucosal involvement affected the oral, ocular, and genital surfaces. Symptoms occurred approximately two weeks after initiation of amoxicillin, dexchlorpheniramine maleate, dexamethasone, and mefenamic acid for an upper respiratory tract infection. Laboratory evaluation revealed mild anemia, hypoalbuminemia, and electrolyte imbalance. The SCORTEN at admission was 1, corresponding to a predicted mortality of 3.2%. All suspected medications were discontinued immediately. The patient received intensive supportive care, multidisciplinary management, and early high-dose systemic corticosteroids. Rapid clinical improvement was observed, with cessation of new blister formation, progressive re-epithelialization, and complete remission without sequelae at follow-up.
This case underscores that TEN may occur in adolescents following exposure to commonly prescribed medications and may present with extensive mucocutaneous involvement without internal organ failure. The presence of multiple potential culprit drugs may complicate etiological identification, representing a diagnostic challenge. Early recognition, immediate withdrawal of suspected agents, and comprehensive supportive management are critical to achieving complete recovery and preventing life-threatening complications.
